Third Time’s the Charm: Sarah Gets Ready to Go Bald Again
It’s been over three years since 2012 Ambassador Sarah has seen herself bald. She’s breaking that streak on Saturday to be a shavee℠ for the third time. As a childhood cancer survivor, Sarah writes about what bravery looks like to her and what makes shaving so special this time.
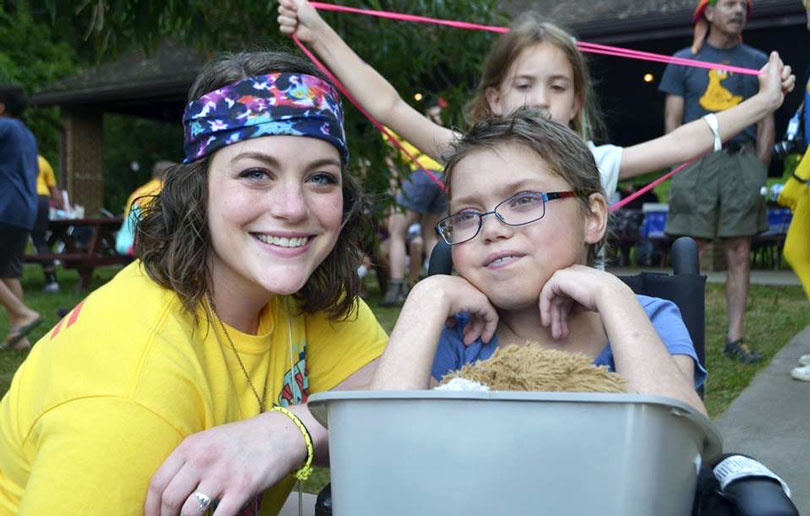
Sarah (left) smiles with Honored Kid Abby at Camp Fantastic in 2015.
I’m often asked if I’m nervous about my upcoming shave.
I can honestly say I’m not at all. After all, this will be my third time shaving my head for the St. Baldrick’s Foundation!
The usual response I get is, “You’re so brave.” But I don’t see myself as the brave one.
Divided, Yet Never So United: Our Family’s Continuing Journey With Childhood Cancer
Today Abby turns 9, and for the second year in a row, she’s celebrating her birthday in the hospital. Her mom, Patty, reflects on the past year and all the challenges their family has weathered together, from relapse to transplant to today.
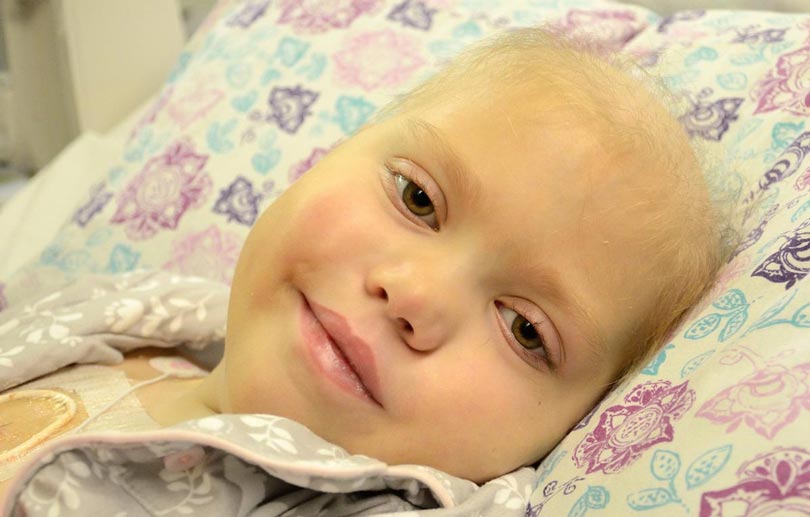
Abby last November, two months after her relapse.
Looking back at where we have been, the many states of mind and motions we have experienced … it’s enough to make my head spin.
Team of Researchers Targets DNA to Help Kids With Hard-to-Treat Leukemias
They say two heads are better than one — what about lots of heads? Thanks to a St. Baldrick’s Consortium Grant, six teams of brilliant minds are working to give hope to kids with hard-to-treat leukemias.
Fifty years ago, the most common childhood cancer, acute lymphoblastic leukemia (ALL), was one of the deadliest.
Cure rates have gone from near zero in the mid-1960s to about 90% currently. That’s amazing, said St. Baldrick’s researcher Dr. Stephen Hunger of The Children’s Hospital of Philadelphia, but it’s not enough.
An Update on Abby [PHOTO ESSAY]
At this time last year, one of our Honored Kids had a new lease on life. (You may remember her from this adorable video.)
At age 4, Abby was diagnosed with an aggressive childhood cancer called Ph+ acute lymphoblastic leukemia. Thanks to research funded by St. Baldrick’s, she went into remission.
But this fall, Abby’s cancer returned. She’s having a bone marrow transplant today.
Here’s an update on Abby.
This summer, Abby completed a kids triathlon.

St. Baldrick’s Researcher Tests New Treatment for Graft-Versus-Host Disease
Dr. Choi, a St. Baldrick’s Scholar, completed a phase II clinical trial testing a new drug to help kids with leukemia and other childhood cancers, and the results are encouraging. Help fund research like Dr. Choi’s. Get involved.
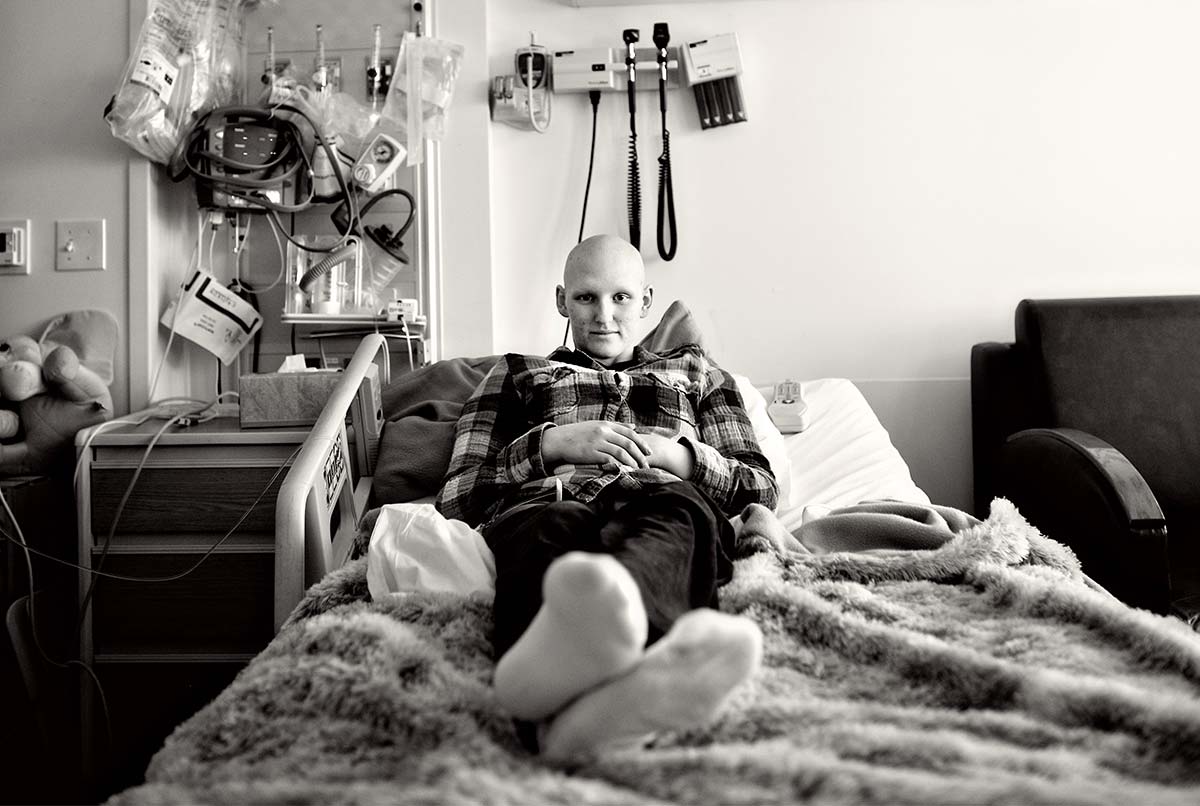
Kids with leukemia, like 2011 Ambassador Julia, sometimes have to undergo a stem cell transplant as part of their childhood cancer treatment. Graft-versus-host disease is a common complication of transplants.
For some kids with cancer, a stem cell transplant is their only hope for a cure. But stem cell transplants are very risky procedures. About half of all transplant patients will experience acute graft-versus-host disease, or GVHD, an often fatal complication where the transplanted immune cells attack the patient’s body.
Life After Chemo: Hope, Faith, and Big Steps
After Abby completed treatment for childhood cancer, her mom had to adjust to a new “normal.”
What do we do now?

Abby was diagnosed with Ph+ acute lymphoblastic leukemia, an aggressive form of childhood cancer, when she was 4.
After doing that daily — along with a whole host of different treatments — for the last 32 months, it’s scary to stop.
We are extremely thankful for what we have and that we still have Abby here with us. But to say that we are celebrating every day isn’t true. At times I find myself holding my breath and waiting.
Every time I hear her coughing or complaining of something, my mind goes all over the place. For the past almost-three years, it’s never been just a cold; it was usually pneumonia. It never was just a tummy ache; it was C. diff, rotavirus, typhlitis, you name it. And now, without the safety net of chemo, is it the dreaded “R-word” — relapse?
We Had a Choice: Abby’s Fight Against Ph+ Acute Lymphoblastic Leukemia
“Your child has cancer.”
When Abby was 4, she was diagnosed with Ph+ ALL, a rare and aggressive form of childhood cancer.
“What do we do now?” began on February 16, 2011, but it didn’t stop that day when our 4-year-old daughter, Abby, was diagnosed with pre-B acute lymphoblastic leukemia (ALL).
“Every child is different, every disease is different, but this is relatively good news,” explained the doctor. “ALL is one of the most common forms of leukemia, and great advances in treatment have been made.”
One week into chemotherapy treatment, Abby’s diagnosis got more complicated when we learned she had Philadelphia chromosome positive (Ph+) ALL, an aggressive subtype of leukemia. Our oncologists let us know that the recommended care would involve a bone marrow transplant.
Update on Ambassador Zoe, the Cancer-Fighting Dancer [VIDEO]
Zoe, a 2010 St. Baldrick’s Ambassador, was diagnosed with Ph+ ALL when she was 4 years old. Now 9, Zoe is starting fourth grade, taking hip hop and ballet classes, and is starting treatment with a targeted chemotherapy pill. Zoe’s mom, Suzanne, gives us an update.

2010 St. Baldrick’s Ambassador Zoe with her mom, Suzanne. Zoe recently started treatment for a molecular relapse due to Ph+ ALL.
When I think of all the things Zoe has seen and done in her life, it is hard to believe she is only 9 years old.
When Zoe was 4, she was diagnosed with acute lymphoblastic leukemia. At first we were told it was the best-case scenario, that leukemia had great treatments and outcomes.
Eight days later, that all changed.
Goodbye Cancer. Hello 3rd Grade.

Zoe was four at the time, and had started limping. My animated, lively daughter, who once turned hallways into runways, was hardly moving. It was a complete, dramatic shift – something I knew was more than just growing pains.
And it was. In 2008, my sweet girl was diagnosed with acute lymphoblastic leukemia (ALL), the most common form of childhood cancer. “She has good odds,” they told us. Survival rates are high for this type of cancer and she should be able to continue most of her normal activities during treatment. We were shocked, but full of hope.
Eight days later, we received a second set of news. And this time, it was worse.
« Newer Posts

 SBF
Tweets »
SBF
Tweets »