
What is medulloblastoma?
Medulloblastoma is the most common malignant brain tumor in children. It originates in the back part of the brain called the cerebellum. In up to 1/3 of cases, it can spread to other parts of the brain and spinal cord. Most cases are diagnosed before age 10.What are the signs and symptoms of medulloblastoma?
The tumor usually blocks normal fluid movement around the brain, resulting in a buildup of fluid and increased pressure in the skull. As a result, patients often experience:- Headaches
- Vomiting (often in the morning)
- Sleepiness or lack of energy
- Changes in vision
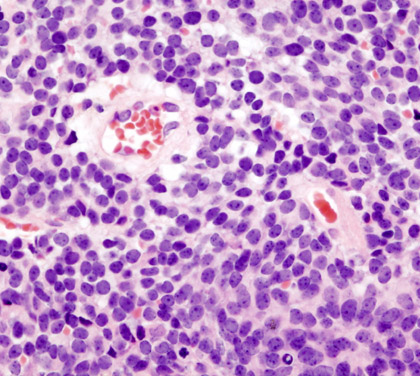
Medulloblastoma cells. Photo via Wikimedia Commons.
How is medulloblastoma diagnosed?
The tumor is initially diagnosed with a CT scan or MRI of the brain. Doctors will then obtain a sample of the tumor through a biopsy procedure or surgery to remove the tumor. A pathologist will then look at the tumor sample under the microscope to determine if it’s medulloblastoma or another type of childhood cancer, or if it’s benign (non-cancerous).What treatment options are available for children with medulloblastoma?
The first step in designing a treatment plan for a child with medulloblastoma is determining whether the tumor is in one place or if it has metastasized, or spread. If the tumor is in one place, the best results for cure begin by removing most or all of it by surgery. This is followed by chemotherapy and radiation treatments to the brain and spinal cord. For patients younger than 3, the long-term side effects of radiation are severe, so doctors usually try to avoid it and instead use stronger chemotherapy. If there’s evidence that the tumor has spread, surgery is still helpful as are radiation and chemotherapy, but metastatic disease is much harder to treat and generally has a poor prognosis.How is research helping children with medulloblastoma?

Dr. Petrosiute at work in the lab.
Join us today and #DFYchildhoodCancers!
Read more on the St. Baldrick’s blog:
 SBF
Tweets »
SBF
Tweets »