This was written by Hudson’s mom, Jessica McKearney.
I work as a Nurse Practitioner and Kyle works as a Project Manager. We live in a small town in Northeast Iowa. Before March 2019, Hudson was an energetic, Mickey Mouse and car loving toddler. He was spirited, happy, loved to dance and kept us on our toes. In November 2018, Hudson became a big brother to his sister Violet. Two under two was exciting and exhausting. Hudson was caring, empathetic, and always wanted to be with Violet. They had an incredible bond, and we were grateful to have two happy and healthy toddlers.

That November, we had photos taken of the kids and I noticed that Hudson looked sick.
In January 2019, both kids came down with a viral illness, RSV, which was Hudson’s first real illness. Both healed with over-the-counter treatment but then, about a month later, I noticed darkness under Hudson’s eyes and purple dots on his forearm. My stomach sank. He hadn’t had any recent injuries that would cause this type of bruising. Working in health care, I knew these were called petechiae, and can happen when a person has low platelets. It’s also a warning sign for leukemia.
I texted my husband and told him, “I think Hudson has leukemia.” I tried to tell myself that kids can get petechiae due to other illnesses, but I couldn’t shake my motherly intuition. Hudson also began having low-grade fevers every night.
I took him to our pediatrician’s office and requested bloodwork to rule out leukemia. Fortunately, we had a provider who validated my feelings. She knew I was an anxious mother and wouldn’t let this go.
An hour later, the phone call came. “Jessica, where is the baby? Are you holding Violet? Hudson’s labs came back. They’re abnormal.” This was the moment everything changed.
How was this possible? He had been fully vaccinated, exclusively breastfed, no daycare, minimal exposure, healthy parents. My son, who was dragging pudding across the floor, was sick. The provider rattled off his lab values. His hemoglobin was 5 and anything less than 8 typically requires a blood transfusion. His immune system function was essentially nothing. His platelets (cells that help us clot) were less than 20, which makes sense considering he had petechiae. I spent my next moments screaming on the phone, “Hudson can’t die. He cannot die. If he dies, I will die.”
She told me to head to the eleventh floor of the University of Iowa Stead Family Children’s Hospital. Immediately, Hudson had an IV in his arm and I was signing consents for a blood transfusion. The oncologist told me that although this could be an autoimmune disorder or virus, this looked very much like leukemia. I felt my entire body stop working. He told me calmly and confidently he would do everything in his power to save our son. And so, our cancer journey began.
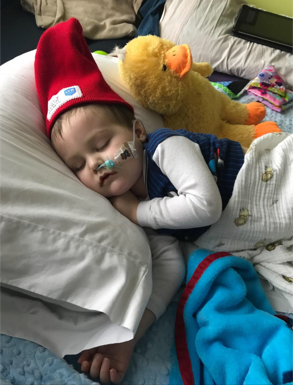
.
That night Hudson received three blood transfusions and two platelet transfusions to stabilize blood counts so he could have procedures to implant a port, do a bone marrow biopsy and lumbar puncture. Results showed that Hudson’s bone was 49% leukemia cells. He was only 23 months old, and his bones were filling with cancer. (Most children have close to 100% of cancer cells in their marrow at diagnosis, because this type of leukemia spreads rapidly.)
His spinal fluid showed possible leukemia cells, requiring more lumbar punctures and more chemotherapy injected into the fluid around his spinal sord. Hudson’s genetics, blood bone and spinal fluid results classified him as “standard risk” B-Cell Acute Lymphoblastic Leukemia. His protocol would consist of nine months of frontline treatment followed by years of maintenance treatment.

.
Fortunately, after a month of steroids, lumbar punctures and IV chemotherapy Hudson was in remission. He spent his second birthday unable to walk or talk because of pain and weakness. The Hudson we had always known was gone. His personality, spirit, happiness, energy, and life seemed to completely darken. We mourned the Hudson we thought would never return but told ourselves we would love the new version just the same.
A few weeks into treatment, Hudson started losing his hair. This crushed me. I caught Kyle removing a pillowcase one morning in Hudson’s bed, trying to shelter me from a pillow full of Hudson’s beautiful hair. It began to fall out onto his shirts, in my hand when rubbing his head and on my lips when giving him kisses. Eventually, the rest of his hair fell out.

.
So much of our days were spent inpatient. We became pros at pushing a toddler, a baby and an IV pole. I had to replace my sons’ NG tube multiple times. My husband held him down while I inserted the tube. Hudson was terrified and begged me to stop torturing him. It had to be done. He needed his chemotherapy and medications.
In November 2019, Hudson hit the maintenance phase of treatment. We thought it would get easier but were wrong. In early 2020, a common virus almost killed him. This reminded us that not only did we have to worry about the cancer taking our son, but also a common illness.
He continues to be treated for leukemia and is scheduled to finish treatment in May 2022. More than half of his precious life has been spent in cancer treatment. Cancer has stolen so many memories, possibilities, birthday parties, and family events.

In his four years of life, he has endured more than most will in a lifetime. The anxiety, PTSD and fear he now has because of treatment is heart wrenching. Instead of playing doctor like a normal kid, he pretends to access a port and perform a lumbar puncture. Despite everything, his strong-willed spirit continues to shine through and show us what true bravery, love, empathy, and resilience looks like. We are so honored to be Hudson’s and Violet’s parents and to witness the kind of warriors they are.
Research for our children is significantly underfunded. Most of the chemotherapy drugs that Hudson has received have been around for decades, some even dating back to the 1950’s. The length of treatment, harsh side effects and late effects could all be improved if we had more research. Many chemotherapy drugs put children at risk for developing cancers later in life. If kids survive the cancer itself and the chemotherapy medications, there are still significant effects later.
As of now, most of these cancers do not have a known cause or risk. Research could lead to a better understanding of those at risk, earlier detection, and more efficient treatment protocols. Without these funds, kids will continue to endure unnecessary pain and late effects. These kids deserve a fighting chance. By getting involved in fundraising for research through St. Baldrick’s, people can help with new treatment discovery, more effective medications, options, and hopefully one day a cure.
Donate now and help support research into better treatments for kids with cancer.
Read more on the St. Baldrick’s blog:

 SBF
Tweets »
SBF
Tweets »